My First Benlysta Infusion
At 7:45 a.m., I approached the medical staff stationed outside my doctor's office to have my temperature taken. My husband had just dropped me off for my first infusion treatment because I was nervous about whether or not I'd be able to drive home afterward.
Starting my infusions during COVID-19 wasn't ideal, but it was important for my health. Wearing my face mask and carrying my coffee (and a fair amount of tension), I got the okay to go inside and check in.
I filled out a short form in the waiting area, barely finishing it before being called back. My nurse was a kind, competent, and straightforward woman – precisely what I needed as I walked anxiously toward the infusion suite. I had to step on the scale, as intravenous (IV) Benlysta dosage is determined by weight.
Getting comfortable before my Benlysta infusion
As the day's first appointment was at 8 a.m., I was given my pick of the 3 available chairs. I settled into a comfortable, blue reclining chair. The nurse took my vitals and gave me Claritin and Tylenol to prevent an allergic reaction, reduce possible fever, and help with the common post-infusion headache.
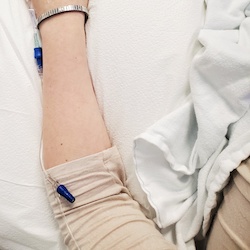 I steeled myself for the next step. I have a phobia of IV lines, which is one reason why I put off infusion treatment for so long. But the nurse put in my IV quickly and then hung the saline I had requested - another headache prevention method.
I steeled myself for the next step. I have a phobia of IV lines, which is one reason why I put off infusion treatment for so long. But the nurse put in my IV quickly and then hung the saline I had requested - another headache prevention method.
The saline ran for nearly 40 minutes, which was how long it took to get my Benlysta mixed up and ready. My nurse hung the Benlysta bag at 8:45 and told me it would take about one hour to finish.
Sitting through my Benlysta infusion
I sat with my hand gingerly, resting on a pillow, since the IV line was causing enough pain in my hand that I didn't want to move it. I decided to have the IV placed elsewhere in the future. The line was taped along my upper arm so it wouldn't be in the way.
 My hand and forearm felt cold from the solution, so I asked for a blanket to help stay warm. I also got an extra pillow for my head, and was quite comfortable overall.
My hand and forearm felt cold from the solution, so I asked for a blanket to help stay warm. I also got an extra pillow for my head, and was quite comfortable overall.
I was relatively relaxed, using my free hand to reply to a few emails, listening to a podcast, and carefully drinking my coffee. I was grateful to lower my mask for eating and drinking briefly.
At 9 a.m., the second infusion patient arrived, and I gathered that the nurse needed most of an hour to get each patient set up (the third patient arrived at 10 a.m.). Even though it was tough to do the 8 a.m. slot, it was a good choice for my first infusion since it meant I got the room – and the nurse – to myself for an hour. I had plenty of time to express my concerns and ask questions.
Halfway through my infusion, I made a bathroom run, awkwardly pushing the IV pole down a long hallway. Trying to do everything with just one hand was difficult as I wasn't dressed accordingly.
By 9:50 a.m., my infusion bag was empty; the nurse flushed out the IV line and removed it. It was simple and quick, and I was surprised to be walking out of the building so soon.
After my Benlysta infusion
I was tired when I got home from the infusion, but not overly so. I would have been just as tired from anything that required me to be out and about that long. I had to ice my hand as it was bruised pretty badly from the IV line, and I couldn't use it for most of the day.
I did have a headache that night and the next morning, and I also felt extra tired the next day. Overall, I felt the infusion was a success and not as hard on me as I expected. Despite my fears, I was proud of myself for going through with it. My next loading dose was in 2 weeks, and I knew I’d be much calmer now that I knew what to expect.
Join the conversation