CPAP Therapy: An Unpleasant Solution for My Fatigue Problems
Sometimes, taking responsibility for your health kind of sucks. Have you been there – where you just want to do the right thing for your health but the process feels horrible? For example, getting nausea from an immunosuppressant, despising a dietary change, or flaring because a new medication doesn’t work well.
Over the years, I’ve had rough side effects and painful tests here and there, but nothing that I found unbearable long-term until now. One of my most recent health treatments has felt almost impossible to keep up with because I hate it so much.
Asking for answers on fatigue
Earlier this year, I brought up my severe fatigue to my rheumatologist for the umpteenth time. She’d already explained why fatigue can be a particularly tough aspect of lupus to treat, but this time I had a new symptom: sleep paralysis.
I find it helpful to bring up new and different angles of my ongoing health issues; it increases the chances of having that aha moment. I described the alarming sleep paralysis I’d been experiencing, but I didn’t love what my doctor said next. She worried that my fatigue went beyond lupus, and wanted a sleep study to check for sleep disorders before proceeding with any other treatments.
My sleep study
I put off making the call to sleep medicine for a few months but finally accepted that I had to do it. The sleep study itself didn’t seem terrible: arrive at 8 p.m. with anything you need to sleep, be set up in bed an hour later, and leave around 6 a.m. the following morning.
I checked in, and the room was surprisingly similar to a hotel room. I got changed and filled out some forms. Then the sleep tech took me to the prep area and put way more stuff on me than I expected. There was goop in my hair to hold electrodes, tape on my face, wires going down into my clothes to attach to my legs, and a monitor up against my nose.
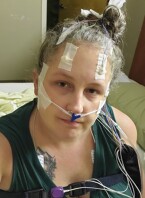
Thankfully I had been given a sleep aid for the night. I took my bedtime meds, did a few checks with the tech to make sure everything was working, and then started to meditate because I was having trouble staying calm.
The next thing I remember is being woken up to have CPAP (continuous positive airway pressure) mask put on my face. It hadn’t been long at all, maybe 2 hours, so I knew I must have sleep apnea. This is one advantage of going into a center to do a sleep study vs. a home test as the staff can try out solutions if they observe a sleep disorder.
Dealing with panic
I sat up, drowsy, trying to follow the instructions from the sleep tech for the CPAP machine. I hadn’t been breathing through my nose at all, so I was given a full face mask (I have since gone to an ENT to find out why and I’m getting my nose problems fixed soon).
Cue the claustrophobia and panic.
Not only did I have to put a large mask on my face, but the forced air made me feel like I couldn’t breathe out. The tech had to lower the air pressure significantly for me to tolerate it. It took a lot of meditation and a few more breaks from the mask before I go back to sleep.
It turns out the CPAP therapy treated my moderate sleep apnea very well during the study. So my doctor ordered a machine.
CPAP machine drama
I had a basic understanding of CPAP machines and sleep apnea from my Dad, but I didn’t know that I would have to wear the machine for 4 hours at least 70 percent of the time for insurance to pay for it - and it’s quite expensive. I had no idea how I’d tolerate it and get the coverage I needed.
I tried using melatonin to help me sleep when I got my machine. My husband sat with me for several nights while I panic-sobbed and kept having to take the mask off. I did "desensitization training," which made me hate the mask more. Finally, my sleep doctor sent a script for a few weeks of sleep medication to help.
With a lot of work, I got to where I could tolerate the mask while falling asleep. But whenever I woke up, I’d panic again and have to get it off my face as soon as possible.
I keep trying because of the health benefits
Treating sleep apnea has tremendous benefits. I’ve been more alert, and calmer, and my blood pressure has come down so much that I’ve reduced my blood pressure medicine by more than half in only 6 weeks.
It’s also been easier for me to concentrate, and I have more energy to exercise. All that happened even though I’m struggling to comply with CPAP therapy, and I’ve used it, on average, 50 percent of the time.
During my sleep study, I had apneas (breathing pauses) up to 20 times an hour. And when my breathing paused, my oxygen would dip as low as 84 percent. That is quite bad for my body. It stresses my heart, and the oxygen deprivation generally leaves me with a morning headache. I’m sure it didn’t help with my lupus, either.
So each night, I sit down next to the machine, which I still loathe greatly, and give myself a little speech about why I’m putting myself through this experience. "It’s for my health. I’ll feel better if I use it." I hope not to need the machine one day, but in the meantime, I will keep doing my best to improve my health even though it’s unpleasant.
What is something you do for improved health that you do not enjoy?

Join the conversation