Lupus Eye Complications
Reviewed by: HU Medical Review Board | Last reviewed: January 2020 | Last updated: August 2022
About one-third of people with lupus develop some sort of complication involving the eyes or the skin around the eyes.1 Eye and vision complications may be caused by the disease itself or by some of the drugs used to treat lupus. Eye complications range from mild and slightly irritating to severe enough to cause blindness. Eye symptoms are often one of the first signs of lupus.
What are the most common eye complications in lupus?
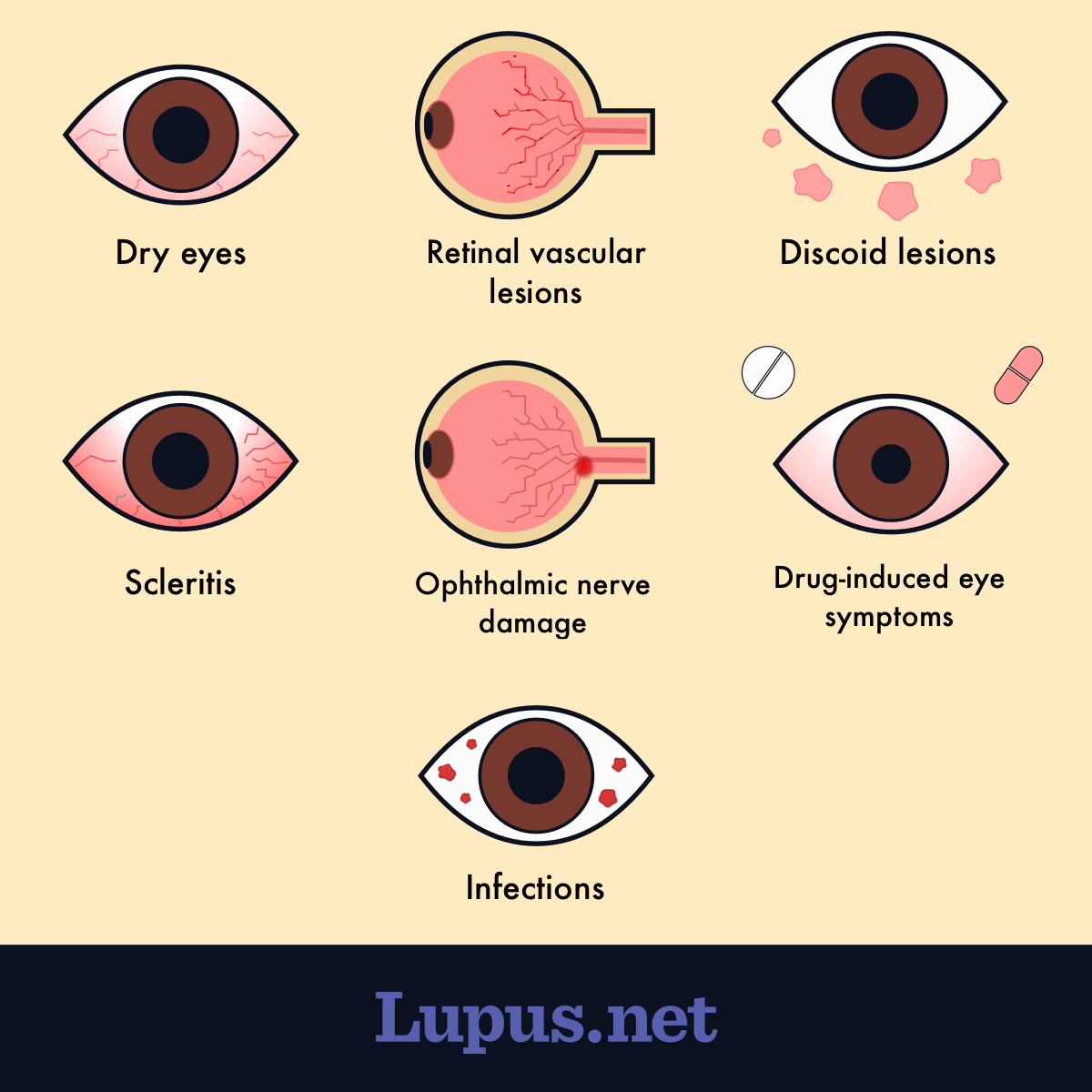
Figure 1. An infographic illustrating common eye complications associated with lupus.
Dry eyes
Dry eyes often feel irritated, gritty, scratchy, or burn, and cause watery eyes and blurred vision. About 20 percent of people with lupus also have Sjogren’s syndrome, a condition in which the glands that make tears and saliva do not work properly. This creates dry mouth and dry eyes. If the eyes are left very dry for a long time, it can damage the front surface of the eye and reduce vision.2
Retinal vascular lesions
These lesions are the most common type of eye symptom, occurring in 3 percent to 28 percent of those with lupus. It seems to be more common in the later stages of the disease. Blood vessels in the retina become damaged by blood clots or inflammation, limiting blood supply to the tissue. This causes mild to a severe loss of vision, that can be temporary or permanent.2
Discoid lesions
Discoid lesions on the skin around the eyes usually look well-defined around the edges, slightly raised, and scaly. These lesions may look unattractive, sometimes cause burning and itching, and can lead to scarring around the edge of the eyelids. This symptom most often appears in people with the discoid form of cutaneous lupus.2
Scleritis
Scleritis, or inflammation of the white tissue of the eyes, is painful and red.2
Ophthalmic nerve damage
The nerves in and around the eyes, called the ophthalmic nerves, may be damaged by inflammation, causing double vision, poor eye movement or alignment, droopy eyelids, vision loss, or visual hallucinations.2
Drug-induced eye symptoms
High doses of the antimalarial drug hydroxychloroquine can be toxic to the retina. People taking hydroxychloroquine should get a baseline eye exam before, or soon after, beginning the drug, and regular eye exams as long as they take it, to monitor for retinal damage.2 Steroids can affect the eyes such as the development or worsening of cataracts. Other immunosuppressants can also cause eye complications.3
Eye infections
Eye infections such as conjunctivitis can be a problem for people with lupus if they are taking immunosuppressants. These drugs make a person more vulnerable to infections of all sorts.
How are eye complications of lupus diagnosed?
Most eye complications of lupus are diagnosed during a physical exam, either by a rheumatologist or an ophthalmologist (a doctor who specializes in eye care). Tests that may be used include:4
- Schirmer test to measure tear production
- Rose-Bengal stain to identify cornea injury
- Slit lamp exam to judge damage and dryness
How are eye complications of lupus treated?
Regular eye exams can help your doctor spot serious complications early enough for successful treatment. The type of treatment will depend upon what type of symptoms you are having. Most eye complications of lupus are treated by controlling lupus itself using antimalarials, steroids, and immunosuppressants.1
In addition, dry eye is treated with over-the-counter eye drops or prescription eye drops that increase the amount of wetness on the eyes. Humidifiers and eye shields may also help combat dryness.4
Drug-induced eye symptoms are treated by reducing the drug in question if possible.3 Eye infections may be treated with a topical (skin cream or ointment) or systemic (pill) antibiotic.3